
Summary EpidemiologyAnnual incidence has been estimated between 1/35,000 and 1/50,000 births and 95% of cases occur in males. Clinical descriptionPrune belly syndrome often presents antenatally on routine ultrasound with oligohydramnios and a very large, distended bladder, mild to severe bilateral hydroureteronephrosis, fetal ascites and occasionally renal dysplasia (see this term) and a patent urachus.
Other anomalies include cryptorchidism, pulmonary hypoplasia, club foot and features of Potter sequence including wide-set eyes, flattened nose, receding chin and large, low-set ears deficient in cartilage. The syndrome is associated with pulmonary, skeletal, cardiac, and gastrointestinal defects and may be associated with atresia of the urethra (see this term).
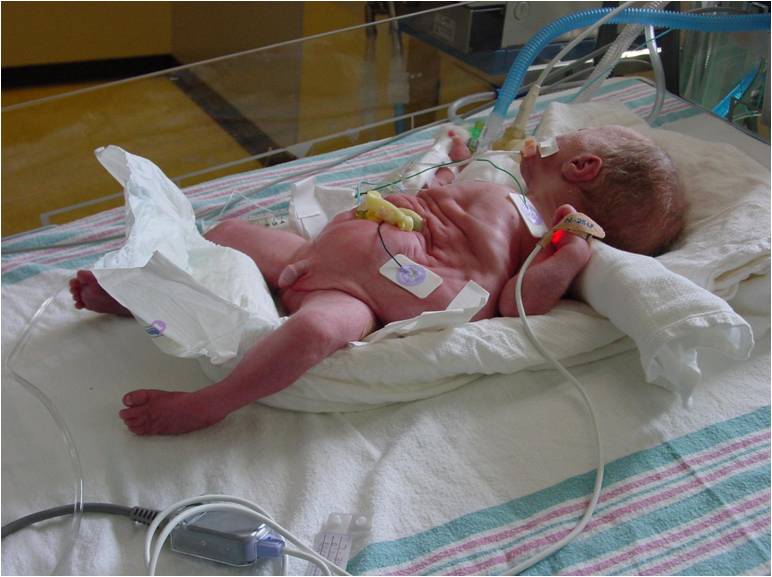
Newborns present with a wrinkled abdomen that later develops a 'pot belly' appearance. There is a predisposition to urinary tract infections due to incomplete bladder emptying in children. EtiologyThe exact mechanism is still unknown; it is thought to arise from urethral obstruction early in development causing massive bladder distention and urinary ascites that leads to underdevelopment of the abdominal wall musculature and failure of testicular descent. The impaired elimination of urine from the bladder also leads to oligohydramnios which in turn affects the development of the lungs resulting in features of Potter sequence. Congenital obstruction of the urinary tract at a critical time in organogenesis may have a profound and lifelong effect on kidney, ureteral and bladder function.
Aug 06, 2019 Prune belly syndrome (PBS), also eponymously referred to as Eagle-Barrett syndrome, is a rare multisystem condition typically characterized by deficient or absent abdominal wall musculature, bilateral intra-abdominal cryptorchidism and urinary tract anomalies including megalourethra, megacystis, hydroureteronephrosis and renal dysplasia. General Discussion. Prune-Belly syndrome, also known as Eagle-Barrett syndrome, is a rare disorder characterized by partial or complete absence of the stomach (abdominal) muscles, failure of both testes to descend into the scrotum (bilateral cryptorchidism), and/or urinary tract malformations.
In cases of siblings with Prune Belly Syndrome and mosaicism, a genetic etiology has been suggested but the majority of cases are of a sporadic nature. Diagnostic methodsDiagnosis is usually antenatal. Postnatal diagnosis is based on characteristic clinical findings, assessment of pulmonary function, ultrasound and voiding cystourethrogram. Differential diagnosisDifferential diagnoses in utero include megacystis/megaureter or posterior urethral valves.
Antenatal diagnosisAntenatal diagnosis is based on ultrasound findings. As with all forms of LUTO, counseling includes a variability of postnatal effects including profound pulmonary hypoplasia due to oligohydramnios and in utero demise to the classic findings of Triad Syndrome without renal compromise.
Genetic counselingAutosomal dominant and X linked inheritances have been observed. Majority of the cases are sporadic, however siblings who are affected have been observed. Management and treatmentSonographic monitoring of the urinary tract and amniotic fluid volume is required throughout pregnancy. Early decompression of severe bladder outlet obstruction that contributes to oligohydramnios is advised. Antibiotic prophylaxis is started at birth with further treatment including bilateral orchidopexies and possible abdominoplasty in addition to potential urologic reconstructive surgery. PrognosisPrognosis depends on the degree of dilation of the urinary tract and the degree of renal functional impairment.
Outcome is typically good in cases with normal amniotic fluid volume. Profound urinary tract obstruction, such as urethral atresia, will lead to progressive oligohydramnios, pulmonary hypoplasia and death in the neonatal period. The most common postnatal cause of death is urosepsis. On the other hand, there are children with normal growth and renal function even though the urinary tract has a markedly abnormal radiographic appearance.Expert reviewer(s): Dr Michael CARR - Last update: January 2015.

